
A hand to hold: Compassion and communication are critical medicines for palliative care physician Mary Raven
Danika Mills was unsure and scared upon realizing she would have to make end-of-life decisions for her mother-in-law, Fabiola Mills. Fabiola, 78, was hospitalized and intubated at Our Lady of the Lake Regional Medical Center this spring after contracting COVID-19.
Fabiola’s adult children, Kermit Mills and Tera Greene—husband and sister-in-law to Danika—were also hospitalized with the disease and fighting for their lives. The decisions about how to ensure Fabiola remained pain free and whether to keep her on life support were left to Danika. Even though she was an ICU nurse herself, Danika wondered if she was making the right choices.
She turned to Dr. Mary Raven, an internist and palliative care physician, for direction. Raven provided daily medical updates about Fabiola and spent hours answering questions and explaining her care plan to allow Danika to make the best possible decisions. “Dr. Raven was like that little angel on your shoulder saying ‘trust yourself,’” says Danika. “I can’t stress how much peace she gave me.”
When the time came to discuss taking Fabiola off life support, Raven arranged a FaceTime call with the extended family to say goodbye because visitors were prohibited in the hospital room. “It was like our private moment,” says Danika. “[Raven] was there, but she wasn’t taking over the moment.”
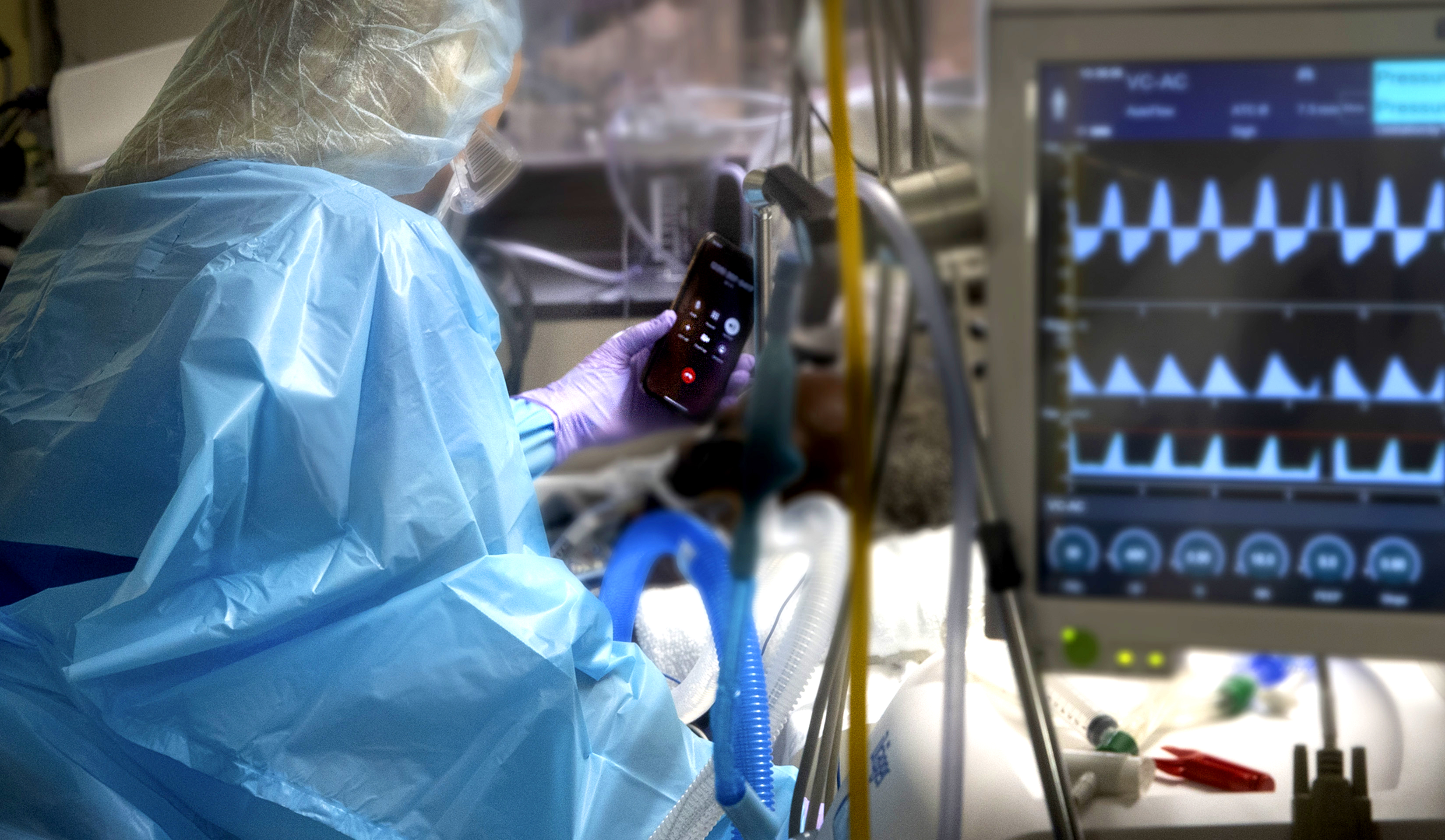
Fabiola Mills died peacefully on April 2, 2020, from complications from COVID-19. “Death isn’t something that is comfortable,” says Danika. “But [Raven] made us all feel like it was OK.”
Although many people associate palliative care with hospice, the specialty aims to optimize quality of life and mitigate suffering among patients with serious illnesses not just at the end of their lives but from the time of their diagnosis. Palliative care can include providing relief from anxiety, depression or the side effects of medicine, Raven says. It also includes initiating difficult conversations with family members to formulate treatment plans and understand goals, she says.
Once patients and their families have a better understanding of what to expect and how to proceed, they make better, more informed decisions, Raven says. “Palliative care has shown time and time again to improve quality of life,” she says.
Although Raven, 41, knew early on she wanted to go into the medical field, she says becoming a palliative care physician was not something she initially considered. “Life just kind of takes you places and you end up where you’re supposed to be sometimes,” she says.
Raven grew up in Rayville and graduated from LSU with a degree in biological sciences. She then attended the LSU School of Medicine in New Orleans and completed her residency in internal medicine at Earl K. Long Medical Center in Baton Rouge, where she also spent an extra year as chief resident.
She decided to become a hospitalist at OLOL Regional Medical Center caring for hospitalized patients. There, Raven wondered why family members didn’t regularly talk to physicians about end-of-life plans for their loved ones and what the patients ultimately wanted. She soon found herself organizing family meetings to discuss treatment plans and answer questions. “It was actually rewarding to see people appreciate that,” she says.
Raven soon met Dr. Mark Kantrow and registered nurse Christine Guidry, who made up the medical center’s small but busy palliative care team. Raven admired the care Kantrow and Guidry provided families and patients and joined the team full time in 2012.
In 2014, Raven and Kantrow established the Outpatient and Palliative Supportive Care Clinic at Mary Bird Perkins-OLOL Cancer Center, the first physician-led palliative care clinic in the state. The clinic started seeing cancer patients one day a week and has now grown to seeing patients four days a week.
Guidry says Raven embodies all of the qualities necessary to excel in palliative care. Raven has the personal resiliency and compassion to meet with families who are often dealing with the worst moment of their lives, Guidry says. “That’s one of the most challenging things,” says Guidry, “bearing witness to the suffering of others.”

Raven’s willingness to coordinate care is tremendous, Guidry says. That means Raven will spend countless hours on the phone reaching out to other physicians or specialists about a patient’s specific needs. “I don’t know physicians outside palliative care who spend that much time coordinating things for their patients,” says Guidry. “It’s part of what palliative care does.”
Not everyone can balance the tough subject matter of palliative care. “It really is something you’re drawn to or you’re not,” says Guidry.
Raven often tells resident physicians they have to be resilient and empathetic if they choose to go into palliative care. “Empathy is that practice of really imagining what another is going through but having enough disconnection to feel the heat from the fire and not be engulfed by flames,” Raven says.
Palliative care physicians must also be able to flip the work/home switch on and off.
At the end of her shift, Raven goes home to her husband and two teenage children. She says her job isn’t more difficult than any other working mom but what helps start her day off right is exercise. Prior to the COVID-19 pandemic, Raven’s workouts used to include swimming three days a week, but now she exercises at home on her Peloton bike or with a friend outside.
The need for palliative care specialists is increasing. Although there is a shortage of palliative care physicians today, the scarcity will hit hardest in a few years when baby boomers, not yet in their 80s, begin to experience a surge of age-related issues, Raven says.
But many young physicians are put off by the potentially depressing aspects of the job. “It’s not a sexy specialty,” Raven says. And palliative care isn’t as lucrative as other specialties. Insurance companies generously compensate doctors to perform surgeries and prescribe medications, but they doesn’t necessarily pay to “talk to people or hold their hands,” Raven says.
During the COVID-19 pandemic, Raven spent nine week straight caring for the sickest patients hospitalized with the virus. Hospital visitation was prohibited, so Raven spent time on the phone with worried family members unable to see their loved ones. Communication without visual cues was an adjustment; when you communicate in person, your body language makes a big difference, Raven says. “People can really see the empathy you convey,” she says. “It’s a little bit easier to establish trust. Over the phone, you have to be very mindful of the words you use to help people understand you do care.”

Several heartbreaking but poignant moments during the crisis stand out for Raven. There was the elderly man with COVID-19 who was isolating at home and unable to visit his sick wife hospitalized with the disease. The couple had been married 50 years, and he was holding onto hope she would survive. When it became clear the wife would not live, Raven arranged a phone call for him to say farewell. When he started talking, it was the first time Raven saw the wife open her eyes in weeks. “It was beautiful,” Raven says.
Then there was the woman who told her hospitalized husband over the phone how grateful she was to be his wife and that she was going to be all right after he passed from COVID-19, Raven remembers. “These are the moments that I and my team were able to participate in, and it was a privilege,” Raven says.
And then there were the Mills and Greene families.
Prior to her mother-in-law’s death, Danika was so impressed by Raven’s bedside manner and personal attention to detail that she asked if Raven would care for her sister-in-law Tera Greene, who was also on life support.
Greene’s daughter, Simone Greene, was equally happy with Raven. “I could tell she really wanted me to be involved, asking questions about the care my mother was getting,” Simone says. “I didn’t feel like I was bothering her or asking stupid questions. She was really there to explain everything every step of the way. I can never repay her for that.”
Tera Greene was released from the hospital after 47 days, including 28 days on life support. Kermit Mills, Danika’s husband, also recovered. The Greene and Mills families say they can never thank Raven enough for her compassion and care. “She really became part of our family throughout all of this,” says Simone. “For all of us, she was the voice we all looked forward to hearing.”











